|
Ask the Doc: Q & A with Edward Kasarskis, MD, PhD
Edward Kasarskis, M.D., Ph.D. is Director of the multidisciplinary ALS Center at the University of Kentucky Neuroscience Center in Lexington, Kentucky, professor in the Department of Neurology at the University of Kentucky, and Chief of Neurology at the VA Medical Center in Lexington KY.
 |
| Dr. Kasarskis |
Q: With spring here, I’m starting to feel the onslaught of hay fever and I find I’m coughing, sneezing, groggy and fatigued, and my eyes are itchy and watery and my nose is running. It’s hard to deal with these symptoms on top of the challenges of ALS itself. What do you suggest?
A: When you hear people complain about their hay fever, they often say, “I’m so stuffed up,” or “I have trouble breathing.” For people with ALS, it’s more than simply an inconvenience. If you’re already having trouble coughing up secretions and swallowing effectively, hay fever or upper respiratory allergies can make you miserable indeed.
To make matters worse, experts are saying that the mild winter temperatures in many parts of the country have caused an earlier-than-usual release of tree pollen, a common trigger for hay fever. And allergists predict a longer and more intense allergy season than we usually have.
ALS complicates hay fever. Depending on your situation, you may have trouble taking in the air necessary to sneeze effectively. Allergies stimulate the creation of secretions, and decreased respiratory capacity can make it difficult to cough deeply enough to clear your lungs and throat. On top of that, some allergy medications can cause drowsiness, which can complicate your breathing when you lie down.
There are some things you can do to feel better:
- The more you can reduce your exposure to allergens causing your hay fever the better you’ll feel. Keeping your windows closed, having a special filter on your heating and cooling system and minimizing the indoor dust and pollen count by vacuuming thoroughly regularly with an allergy-prevention filter may help.
- Keep hydrated to help thin your secretions; they’ll be easier to cough up. Use nasal sprays to moisten your mucous membranes in your nose (although sniffing the sprays depends on your ability to take in a deep breath).
- Talk to your general practitioner or internist about what medications they recommend. Some over-the-counter medications, such as Claritin® (loratidine) treat runny nose, itchy, watery eyes, sneezing, and itching of the nose and throat. Non-drowsy formulas are available and you typically take one 10 mg tablet. Eye drops and nasal sprays are also available.
- Ask your pharmacist to check to be sure any over-the-counter or prescription drugs you may start taking for hay fever and upper respiratory allergies won’t interact with the medications you’re already on.
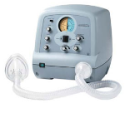 Allergy shots may be an option for you but they typically take several months to be effective. Your doctor may recommend you see an allergist, if necessary. Allergy shots may be an option for you but they typically take several months to be effective. Your doctor may recommend you see an allergist, if necessary.- If you use BiPap, be sure you’re getting humidified air. (Some third-party payers are reluctant to cover the extra cost). The extra moisture will help prevent your nose, mouth and throat from drying out and will make it easier for you to deal with the additional secretions the allergy causes
- Talk with your ALS neurologist and clinic team members about the benefits of using a cough- assist device. It’s a noninvasive therapy that safely removes secretions in people who can’t cough effectively (peak cough flow less than 270 l/m). A cough-assist device clears secretions gradually by applying a positive pressure to the airway, then rapidly shifting to negative pressure, which produces a high expiratory flow, much like a natural cough. It’s easy to use and a good alternative to suctioning; and it can be used with a face mask, mouthpiece or an adapter to a person’s tracheotomy tube. It is not just for the allergy sufferer with ALS, but helpful for many ALS patients at a certain stage of their illness.
Spring has exploded this year in central Kentucky and around the nation. You can take steps to make this allergy season more manageable. I hope you’re feeling better soon!
If you would like to submit questions for a future Q & A, please send your questions to theexchange@alsa-national.org. Please understand that we won’t be able to address all questions and we won’t be able to respond to individuals personally.
|



